8th Postgraduate Course for Training in Reproductive Medicine and Reproductive Biology
Mechanism of Action of Mifepristone and Levonorgestrel for Emergency Contraception
B. Krämer
Germany
Tutor: Dr. Helena von Hertzen
HRP - UNDP/UNFPA/WHO/World Bank Special Programme
Introduction
Emergency contraceptive pills (ECPs) are an important option for women who have recently had unprotected intercourse or a contraceptive accident and who do not want to become pregnant. ECPs have been shown to be safe and effective in studies conducted over the past two decades. The most often used methods of EC are the Yuzpe regimen and postcoital insertion of an IUD [14]. But the efficacy and toleration of established methods for emergency contraceptives have to be improved, and it seems that the two compared methods mifepristone (an Antiprogestogen) and levonorgestrel (a Progestogen) will be approaches because of their higher efficacy and lower incidence of side effects.
Established methods [Ref.1]- High dose estrogen (1963)
- Estrogen-progestogen combination; Yuzpe regimen (1972)
- Intrauterine contraceptive devices (1976)
- Danazol (1982)
- Progestogens (1970) ý future
- Mifepristone (1979) ý prospects
Although there is some debate about its effectiveness, few people question the important role that emergency contraception can play in preventing unwanted pregnancy and maternal mortality and morbidity resulting from unsafe abortion [15].
In April 1995, in Bellagio, twenty-four experts from around the world discussed the fields of emergency contraception. They complained that women and providers are uninformed about the methods, that only few products are marketed for emergency contraception and that service providers are too often reluctant to provide this method. The proposed recommendations include the methods, where they emphasize the antiprogestogens as very promising compounds and that they deserve top medical research priority [16].
For the development of the improved new methods we need more information about the mechanism of action. Probable mechanisms include prevention of ovulation, fertilization or implantation but the exact mode of action is not known [14].
Methods
Mechanism of action
All emergency contraception methods currently in use act before implantation. Theoretically, this could be achieved in several ways; in practice, the possible modes of action are more limited, because women request emergency contraception at different times during their menstrual cycle. This variability in timing means that compounds that work only through disturbing ovulation or some event closely associated with it cannot be highly effective as emergency contraception methods.
Timing of treatment
Because postcoital contraception is given at all stages of the cycle, the mode of action is variable. In the early stages, it may prevent the development of follicle. It is possible, however, that a further follicle will develop without any vaginal bleeding, which may explain the few women whose period is delayed. The main mode of action, however, is thought to be on the endometrium. Changes can be observed which make the environment hostile for implantation. As implantation starts 6 days after fertilization, giving treatment within 72 hours allows at least 2 days for the hormones to have an effect. This would explain the reduced effectiveness if the treatment would be given more than 72 hours after intercourse.
The risk of conception is high between 5 days before and 1 day after ovulation and is highest the 2 days prior to ovulation (Table 1). Even in a woman with reasonably regular cycles, the day of ovulation can vary, and anyone with moderate experience in obstetrics knows of women who have conceived on unlikely days of the cycle. It is therefore best to give EC to all women at risk except when intercourse took place in the first 3 days of normal menstruation or when normal menstruation started before seeking treatment [2] (see Figure 3).
Table 1. Probability of conception based on 129 menstrual cycles in which sexual intercourse occurred on only one day during the six-day interval ending with the day of ovulation and all 625 cycles (Northcaroliner early pregnancy study by Wilcox et al., 1982-1985).
| Day in relation to ovulation |
No. of cycles with intercourse only on this day |
No. of pregnancies |
Single-day conception rate |
Estimated conception rate ± SE* |
| -5 |
12 |
1 |
0.08 |
0.10±0.08 |
| -4 |
24 |
4 |
0.17 |
0.16±0.06 |
| -3 |
13 |
1 |
0.08 |
0.14±0.08 |
| -2 |
28 |
10 |
0.36 |
0.34±0.07 |
| -1 |
38 |
13 |
0.34 |
0.31±0.06 |
| Day of ovulation |
14 |
5 |
0.36 |
0.33±0.09 |
| Total |
129 |
35 |
|
|
*Estimated conception rates are based on maximizing the likelihood under a semiparametric model with the use of data from all 625 cycles.
Figure 1 depicts how a drug’s mode of action influences its potential value as an emergency contraception.
Figure 1. Timing in the menstrual cycle when emergency contraceptive compounds would be effective. Arrows indicate the period of compound’s effectiveness. Drug A blocks oocyte maturation or ovulation. Drug B provides fertilization, Drug C intercepts postfertilization events.
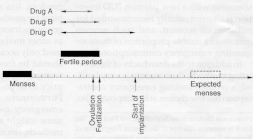
Drug A: It acts during the follicular phase only, by interfering with oocyte maturation or by blocking ovulation. But it would only be effective at preventing pregnancies that result from intercourse in the preovulatory phase, if the treatment is started soon enough before ovulation.
Drug B: It prevents fertilization rather than ovulation and would be a more useful approach, since the window of activity would be wider. This compound should be capable of preventing fertilization, even if both unprotected intercourse and use of the drug take place early in the fertile period.
Drug C: If intercourse were to take place late in the fertile period, at about the same time as or shortly after ovulation, fertilization may not be successfully blocked. Spermatozoa reach the site of fertilization within a few minutes following intercourse [5, Ref.9], and even if the woman were to start treatment shortly after coitus, its almost never possible to achieve an effective drug concentration in time at the fertilization site.
The ideal emergency contraceptive drugs should be capable of interfering with a physiological event that occurs after fertilization, during the period of early embryonic development prior to implantation (see arrow of drug C). It must exert its effect for the entire duration of the fertile phase, including the critical moment in the endometrium preparation for the implantation (nidation), plus the time needed until the targeted event occurs. It may be a drug that combines preovulatory and postovulatory modes of action, to be effective (Ref. International Family Planning Perspectives Research on new methods of Emergency Contraception) [5].
Timing - What the doctor should ask: [2]- First day of last menstrual period
- Length of cycle
- First episode of unprotected intercourse
- Attempts at contraception
Mifepristone
Mifepristone, the generic name of RU 486 is a new class of drugs known as antiprogestogens. It is approved for use in early abortion in a small number of countries (China, France, Sweden and the United Kingdom). Its possible use as an emergency contraceptive is under study, but it has not been approved for this purpose in any country yet [14].
1979 – A research project for the development of glucocorticoid antagonists (11b -substituted steroid) started by the pharmaceutical company Roussel-Uclaf (France). Mifepristone (RU 486) was produced a few months later, and it was found, to possess high affinity not only for the glucocorticoid receptor but also for the progesterone receptor.
Since the discovery of Antiprogestogens, it has been suggested that it has potential value in fertility regulation and in the field of obstetrics and gynecology and possibly also, in other disciplines of medicine [3].
The antiprogesterone drug, mifepristone , is a synthetic steroid that prevents progesterone (and glucocorticoids) from binding to hormone receptors. Because mifepristone can block ovulation or retard endometrial development, depending on whether it is administered before or after ovulation [1, Ref.27], it seemed probable that the compound would be effective in EC. This was confirmed by two randomized trials from WHO, about postcoital contraception with mifepristone [1, Ref.28], and alternative treatments in oral postcoital contaception [1, Ref.29].
To talk about antiprogestogens and its mechanism of action, some information about progesterone can be useful.
Progesterone is involved before ovulation, in follicular maturation and the process leading to ovulation [5, Ref.27]. It is a major constituent of follicular fluid and may be the component responsible for inducing the movement of spermatozoa to the ovum for fertilization [5, Ref.28], it may also produce structural changes that facilitate the entry of spermatozoa into the ovum [5, Ref.29]. It influences the transport of the fertilized egg through the Fallopian tube and causes endometrial changes (known as decidualisation), that are required for successful implantation and establishment of pregnancy. It also affects the function of the endometrial epithelium and the interaction between that surface and its supporting structure (the endometrial stroma)[5].
Progesterone Inhibition
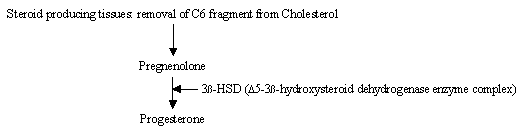
Any substance interfering with the synthesis (Figure 2), secretion or peripheral actions of progesterone has the potential for use in emergency contraception. Compounds that fall into this category include substances that disrupt the corpus luteum, inhibitors of progesterone synthesis and progesterone receptor blockers (antiprogestogens). Compounds with antiprogesterone activity can be grouped into two main categories:
(1) Steroid enzyme inhibitors that prevent the biosynthesis of progesterone at the level of the steroid-producing cells.
(2) Progesterone receptor blockers (designated as "antiprogestogens" in this paper) that interfere with the binding of progesterone to its cellular receptor in target tissues. This category will be of interest, in consideration of Mifepristone.
Figure 2. Biosynthesis of Progesterone
Progesterone-Receptor blockers
Antiprogestogens act directly at the cellular level, by binding to the progesterone receptor and blocking the action of progesterone. Their influence is thus more immediate than that of progesterone synthesis inhibitors. While hundreds of compounds with antiprogestational activity have been identified, only a few have been sufficiently evaluated in biological screening models and only four - mifepristone, lilopristone, onapristone and CDB 2914 (known as HRP 2000) - have been given to humans. Most antiprogestogen research to date has been on mifepristone (RU 486).
Most of the molecules shown to possess antiprogestational activity have a bulky substituent at C-11, usually a dimethylaminophenyl group as found for example in mifepristone. The available preclinical data suggest that there can be marked differences between antiprogestogens in their antiprogestional and antiglucocorticoid activity. No "pure" antiprogestogens have been described to date, and it is not clear if the antiglucocorticoid activity present in currently available antiprogestogens has a modulatory influence- either positive or negative- on the antiprogestional potency. There is an urgent need to separate these two activities.
Confirmed and suggested applications of the antiglucocorticoid property of currently studied antiprogestogens include the palliative treatment of hypercortisolism due to Cushing’s syndrome, certain forms of depression and of glaucoma, and wound healing [4].
Mechanisms of action and effects of mifepristone:
When antiprogestogens are given prior to ovulation, they disrupt the normal sequence of follicular maturation. Depending on the dose and timing of administration, the treatment can cause regression of the dominant follicle and initiate a new cycle of follicle development [5,Ref.31]. However, a low dose may only halt the maturation of the follicle for a short time and, as soon as the antiprogestogen’s influence is over, the same follicle may either proceed to ovulation or remain unruptured until the end of the cycle. For example, a single 5 mg dose of mifepristone given when the leading follicle was 14 mm in diameter retarded the growth of the follicle for up to 36 hours [5, Ref.32]. Data from two studies suggest that to exert a blocking effect on ovulation, the antiprogestogen has to be given before the onset of the luteinizing hormone surge; if the surge has already started, it may be too late to inhibit ovulation with an antiprogestogen [5, Ref.27 u. 31].
Studies conducted to determine whether mifepristone affects fertilization show that if ovulation occurs despite treatment, the ovum appears capable of fertilization. For example, in a study of the effect of mifepristone on in vitro fertilization of human oocytes, the researchers administered 100mg orally 35 hours before recovering the oocytes through laparoscopy (when the follicular diameter was greater than 15 mm) [5, Ref.35]. Although they found substantial amounts of mifepristone in follicular fluid, the in vitro fertilization and cleavage rates of the collected oocytes were not affected. Whether mifepristone could influence the ability of spermatozoa to fertilize in vivo is unclear. Researchers have recently shown in vitro that high concentrations of mifepristone were required to slow sperm movement [5, Ref.36]. Such concentrations are unlikely to be reached in vivo in the tubal fluid.
Apart from affecting follicular maturation and ovulation (and possibly fertilization), mifepristone may prevent pregnancy by influencing the development and transport of embryos. Administration of mifepristone to rats accelerated embryo transport through the tube and caused the loss of embryos from the uterus before implantation. The treatment also delayed or arrested embryonic development [5, Ref.37]. Inhibition of the development of fertilized eggs by mifepristone has also been observed in other species [5, Ref.38]. Whether these mechanisms also contribute to the antifertility effects of mifepristone in the human is not known.
While treatment with mifepristone in follicular phase inhibits follicle development, administration immediately after ovulation significantly affects endometrial maturation. For example, in one study, a 200 mg dose given in the evening of the second day after the luteinizing hormone peak delayed endometrial development for at least six days, even though circulating levels of progesterone were normal [5, Ref.39].
Another study demonstrated the effect of low doses of mifepristone on ovarian function and endometrial development. It showed that low doses, once weekly administered, do not inhibit ovulation but delay endometrial development and impair secretory activity with a prolonged follicular phase by 6-13 days with a normal luteal phase and LH peak [5, Ref.39b].
Furthermore, studies have shown that a single dose of mifepristone administered in the early luteal phase, two days after ovulation, effectively prevented pregnancy in the rhesus monkey, but observed a prolonged cycle length, due to an extension of the luteal phase [5, Ref.41]. In humans, a study with monthly early luteal phase treatment (200 mg mifepristone) for their only contraceptive method has shown similar results [5, Ref.42].
In the latter study, 21 fertile women took 200 mg of mifepristone two days after the luteinizing hormone surge as their only method of contraception; only one pregnancy resulted during 157 cycles. The earlier during the secretory phase that mifepristone is administered, the more marked is its effect on the endometrium. "When the drug was given 2 days after the LH peak, it prevented appearance of the epitope. When Ru486 was administered 5 days after the LH peak, epitope already present in gland cells was subsequently secreted." An examination of doses of mifepristone (from 5 mg to 200 mg), taken from the second until the fifth day after the luteinizing hormone peak, found that the effects on secretory activity of endometrial glandular cells on any given day were essentially similar, irrespective of the dose (5, Ref.47). Another study observed abnormal secretory maturation of the endometrium- considered to be incompatible with successful implantation- after two doses of 10 mg of mifepristone taken 72 hours apart on the fifth day after the luteinizing hormone surge. Cycle length and hormonal patterns were unaltered after treatment [5, Ref.48].
Since Mifepristone appears to be an effective Emergency contraceptive at a dose much lower than those required to induce abortion it may be prove to be valuable and to prevent unwanted pregnancies and recourse to abortion [9, Ref.18]. It has been shown that even a 5mg dose can arrest follicular growth for several days [9, Ref.4]. Further, in the secretory phase of the menstrual cycle, the effect of mifepristone on the endometrium is stronger, the earlier it is given and appears more related to the timing of administration than to the dose [9, Ref.5, 6].
- Reducing the dose of mifepristone may lower the cost
- After lower doses women are less likely to have a delay in the onset of next menses.
Levonorgestrel
Levonorgestrel belongs to the class of Progestogens, it is a synthetic steroid and mostly used as regular oral contraception.
During the 1970`s, a number of studies were undertaken, mostly in South America, to test the efficacy of various progestogens given alone for postcoital contraception (17). Most of these studies examined the potential of progestogens for regular postcoital use, an application for which they were found to be unsuitable, because of the high incidence of cycle disturbances. In EC, such menstrual irregularities are much less of an issue and, in fact, tablets or 0.75 mg levonorgestrel for ‘occasional’ contraceptive use are marketed in several countries.
(see randomized trial from WHO) [1]
The few studies that have looked at levonorgestrel`s mechanisms of action in postcoital contraception suggest that it may affect both follicle growth and development of the corpus luteum (the progesterone-secreting tissue that forms in the ovary immediately after ovulation). One study, in which women received 1.6mg of levonorgestrel on day 10 of their cycle, showed that the treatment seemed to suppress the midcycle luteinizing hormone peak (which induces ovulation), but did not appear to influence the formation and function of the corpus luteum, since the urinary excretion of pregnanediol (the main metabolite of progesterone) was normal [5, Ref.14].
Another study, which examined the effects of a daily dose of 0.75 mg of Levonorgestrel administered for four days either before ovulation, around the time of ovulation or after ovulation, indicated that the impact of Levonorgestrel depends on the time of administration [5, Ref.15]. When Levonorgestrel was given during the early follicular phase, the total cycle length was significantly prolonged due to the increased duration of the follicular phase. Posttreatment biopsies taken on cycle days 20-22 still showed proliferative endometrium in accordance with the delay in ovulation.
When levonorgestrel was administered around the time of ovulation, the effects were variable: Ovulation was blocked in some women, while in others follicular activity was followed by deficient luteal function, and still other women ovulated normally. On the other hand, administering levonorgestrel during the luteal phase did not affect cycle length or cause any significant endometrial changes. This last finding was somewhat unexpected in view of the proven effectiveness of levonorgestrel in emergency contraception [5].
Is Levonorgestrel an improved alternative to the Yuzpe regimen [11]?
In Hong Kong the prospective randomized study was conducted, to compare the efficacy of Yuzpe regimen and levonorgestrel (0.75 mg for two doses 12 h apart, as it is marketed in several countries for occasional use as postcoital contraceptive) in postcoital contraception. The failure rates were nearly similar (2.6 and 2.4%), confirmed with a later randomized study by WHO with the conclusion, that levonorgestrel is an more effective drug for post-coital contraception with a lower incidence of side-effects than the Yuzpe regimen [12,13].
On 1974, a study in South America reported of the hormonal and peripheral effects of d-Norgestrel, a synthetic progestational compound as postcoital contaception. It has been administered satisfactorily in oral doses of 400 micrograms post-coitus, and has yielded a corrected treatment failure rate of 1,7 per 100 woman years of use. The alteration consistently observed in the cervical mucus, with consequent prevention of sperm migration, has been suggested as the principal contraceptive mechanism (table 2, table 3, table 4). However, in postcoital contraception, treatment is applied to prevent conception when coitus already has occurred.
Table 2.Cervical mucus in the ovulatory phase. Effect of a single dose of 400 micrograms d-Norgestrel [6].
| Time after ingestion of dose | Number of patients | Spinnbarkeit cm | Crystallization % |
| Control | 13 | 6.8±0.6* | 79±2.9 |
| 3h | 16 | 4.8±0.6 < 0.05** | 60±5.9 < 0.01** |
| 4h | 10 | 3.2±0.6 < 0.001 | 43±4.7 < 0.001 |
| 7h | 16 | 3.3±0.5 < 0.001 | 31±3.7 < 0.001 |
| 9h | 14 | 3.0±0.4 < 0.001 | 23±5.9 < 0.001 |
| 10h | 29 | 3.0±0.2 < 0.001 | 24±4.2 < 0.001 |
*Mean +/- SE
** Comparison with control group
Table 3. Intercervical sperm penetration. Effect of a single dose of 400 m g d-Norgestrel [6].
| Time after ingestion of dose | Number of patients | Total number of sperm | Number of motile sperm | Sperm with forward motion |
| Control | 13 | 35±5.6* | 27±4.8* | 21±3.1* |
| 3h | 16 | 37±5.3 NS** | 30±4.4 NS** | 20±3.4 NS** |
| 4h | 10 | 40±6.0 NS | 29±4.1 NS | 15±3.4 NS |
| 7h | 16 | 31±4.7 NS | 24±4.7 NS | 15±3.8 NS |
| 9h | 14 | 19±2.7 <0.05 | 14±2.4 < 0.05 | 6±1.7 <0.001 |
| 10h | 29 | 17±1.5 < 0.01 | 11±1.9 <0.01 | 5±1.2 <0.001 |
*Mean +/- SE
** Comparison with control group
Table 4. Recovery of intrauterin sperm. Effect of a single dose of 400 micrograms d-Norgestrel [6].
| Time: Dose to test | Number of patients | Number of positive cases | * |
| Control | 13 | 10 (85 %) | 4.1 |
| 3h | 16 | 12 (75 %) | 2.5 |
| 4h | 10 | 2 (20 %) | 1.5 |
| 7h | 16 | 1 (6 %) | <1 |
| 9h | 14 | 1 (7 %) | <1 |
| 10h | 29 | 2 (7 %) | <1 |
* In positive cases, average number of sperm per LPF.
In Hong Kong the prospective randomized study was conducted, to compare the efficacy of Yuzpe regimen and levonorgestrel (0.75 mg for two doses 12 h apart, as it is marketed in several countries for occasional use as postcoital contraceptive) in postcoital contraception. The failure rates were nearly similar (2.6 and 2.4%), confirmed with a later randomized study by WHO with the conclusion, that levonorgestrel is an more effective drug for post-coital contraception with a lower incidence of side-effects than the Yuzpe regimen [12,13].
Comparative Research Studies
There are four randomized controlled trials of emergency contraception to present as practical part of the discussed treatment regimens to study the efficacy, the timing, and the dose-issue by comparing.
Levonorgestrel versus the Yuzpe regimen (1998)
Methods: double-blind, randomized trial- Levonorgestrel (0.75 mg repeated 12 h later) or
- Yuzpe regimen (ethinyloestradiol 100m g, plus levonorgestrel 0.5 mg, repeated 12 h later)
General informations:
Yuzpe regimen is the most commonly used emergency contraceptive (75% of prevented pregnancies).
Levonorgestrel is marketed in several countries for occasional postcoital contraception in packs containing 0.75 mg tablets.
Discussion
This trial produced two findings of public-health importance.
1. The levonorgestrel regimen was better tolerated than the Yuzpe regimen. Efficacy was greater, in terms of both crude and adjusted pregnancy rates (Lev: 1.1% and Yuzpe 3.2%) and pregnancies prevented (Lev: 85% and Yuzpe 57%). The clustering of observed pregnancies around predicted ovulation (Figure 3) validates our estimates of conception probabilities in this large sample. Because of the biological variability in cycle length and the need to rely on calculated estimates of the day of ovulation, the occasional pregnancy after intercourse apparently outside the fertile period is to be expected.
Figure 3. Observed and expected numbers of pregnancies by timing of coitus.
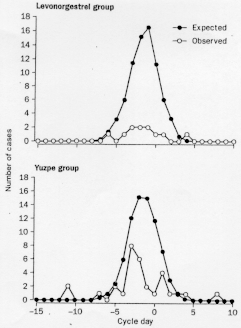
2. The second finding of public-health importance relates to the timing of the treatment. For both methods combined, efficacy was significantly and inversely related to time since unprotected coitus. A trend of decreasing efficacy with time for each regimen was described. Different findings of importance to the timing lead to the proposal that women should receive treatment as soon, as is practicable after unprotected coitus. The sooner treatment starts, the better it works. Neither regimen substantially delayed the onset of next menses.
Mechanism of action: Little is known about, to explain why the Yuzpe regimen of levonorgestrel with ethinyloestradiol is less effictive than the regimen of levonorgestrel alone. The lower efficacy could be due to an interaction between the oestrogen and the progestagen as well as to the lower dose of levonorgestrel used in the Yuzpe regimen.
Replacement of the Yuzpe regimen with levonorgestrel should improve the acceptability of hormonal emergency contraception. [7]
Mifepristone compared with high-dose estrogen and progestogen (1992)
Methods: randomized controlled trial
- 100 m g of ethinyl estradiol and 1 mg of norgestrel, twice 12 hours apart or
- 600 mg Mifepristone
Discussion: Regardless of the method, by which failure rates are calculated, the fact remains that none of the women and adolescents who were treated with mifepristone conceived. It was unquestionably as effective as the standard estrogen-progestogen regimen. Mifepristone was associated with fewer side effects. Since it was taken as a single dose, there was no possibility of noncompliance if side effects occurred.
The only apparent disadvantage of mifepristone was that more of the women and adolescents who took it had a delay in the onset of the next menstrual period – undoubtedly stressful to a woman who was worried that she might be pregnant.
The real problem with emergency postcoital contraception is not its failure rate or its side effects but the fact that so few women and adolescents who have had unprotected intercourse actually use it.
Conclusions: Mifepristone is a highly effective postcoital contraceptive agent that, if used more widely, could help reduce the number of unplanned and unwanted pregnancies. [8]
Three single doses of mifepristone in emergency contraception (1997)
Methods: previous WHO-supported multicentre, single-blind, randomized controlled trial- 600mg Mifepristone within 72h
- 600mg, 50mg and 10mg Mifepristone within 120h
Main outcome measure: confirmed pregnancy
Secondary outcome measures: side effects and the timing of onset of menses.
Findings: The number of pregnancies was similar among women receiving 10 mg, 50 mg and 600 mg , with acorresponding pregnancy rate of 1,2%, 1,3% and 1,3%.
Lowering the dose of Mifepristone sixty-fold did not reduce its efficacy as an EC under typical use. In contrast, lower doses of Mifepristone were associated with no major side effects and less disturbance of the menstrual cycle and, thus appear preferable to the 600mg dose. Mifepristone delays or blocks ovulation if the antiprogestogen was administered in the preovulatory phase of the menstrual cycle [9, Ref.3] Such delay can worry women already fearful of an unintentional pregnancy. It also means conception risk later in this prolonged cycle if no contraception is use.
Comment: Two tubal pregnancies were seen in the study. But no information is available about possible influence of antiprogestogens on tubal transport of fertilized egg in the human, although accelerated transport has been reported in the rat [9, Ref.13] If the woman has already a tubal pregnancy mifepristone does not disturb it [9, Ref.14].
Mifepristone compared with two regimens of levonorgestrel in emergency contraception (1998)
Objective: to compare in a large multinational study, the efficacy and side effects of- 10 mg dose of mifepristone
- levonorgestrel in two doses of 0.75mg at 12 hours interval
- levonorgestrel in one dose of 1.5 mg
Proposed research: administered up to 120 hours after unprotected intercourse
As both mifepristone and levonorgestrel appear to represent an improvement in the methods of EC, it is important to compare these two methods with regard to efficacy and side effects and to see whether they can be effectively used beyond the 72 hour limit since intercourse.
Expected study outcomes: Information from this study will be of value to practitioners providing emergency contraception and, depending on the trial’s outcome, may help the practitioners when choosing the most appropriate method for their clients [10].
Discussion
Mifepristone may be the drug of choice. However, for a variety of reasons mifepristone is still not available in many countries and it is likely that it will remain unavailable for the foreseeable future. On the other hand, levonorgestrel is currently used in different formulations in many countries. In view of lower incidence of gastrointestinal side effects, it is probably a better choice than the Yuzpe regimen.
Because of the political sensitivity surrounding antiprogestogens, it would be an advantage if a very low dose, ineffective to induce abortion, proved to be useful in emergency contraception. It might then be possible, at least in theory, to use the drug for emergency contraception and prevent unwanted pregnancies and abortions also in countries where access to abortion is restricted [11].
Antiprogestogens are not merely "abortion pills", they have a variety of other potential applications in several fields, including fertility regulation. Indeed, the ability to prevent pregnancy may well turn out to be a much more significant characteristic [4]. Most of the research has focused on the use of mifepristone in combination with a prostaglandin analogue for pregnancy termination and most of literature you can find is focused on it.
Research on methods plays an important role for the development of more effective approaches to emergency contraception but new findings from other Research directions should be taken into account. When results from research into mechanisms of action of emergency contraception are interpreted, it should be taken into account, that for example the human endometrium may be morphologically and functionally different during conception cycles than during non-conception cycles. (There is increasing evidence, that the embryo plays an active role in the implantation process, even before implantation, the human embryo produces a number of substances; research in treatment with emergency contraception is done in women, not expose to the risk of pregnancy) [5].
Conclusions
When reviewing the prospects of new approaches to EC, one is forced to conclude that it is likely that basic research into, for example the mechanisms involved in implantation or the regulation of the corpus luteum will yield any new methods in the near future. The currently most pressing need therefore is to continue the clinical evaluation of antiprogestogens for this indication. Compared to current hormonal methods (high-dose estrogen and the Yuzpe regimen), mifepristone has several advantages. It is easier to administer as only one dose is needed, it is more effective and it causes fewer side effects.
In countries where an antiprogestogen-based methods like mifepristone cannot be made available, the use of levonorgestrel may provide a better option to the Yzuspe regimen, if its efficacy is confirmed by future trials [11]. Levonorgestrel is a less ‘controversial’ drug for use in emergency contraception. A main advantage of the levonorgestrel regimen compared with the Yuzpe regimen is the low incidence of side effects especially nausea, vomiting and fatigue [12].
Recognizing the important role that emergency contraception can play in preventing unwanted pregnancy family planning programs, that claim to improve women’s reproductive health, have to provide EC as part of their routine services. Viewed from their perspective, mifepristone has the advantage that it is easier to administer (one dose as opposed to two doses), in addition to having a greater effectiveness and a lower incidence of side effects. The more common occurrence of menstrual delay with mifepristone should not be a major problem if proper counseling and follow-up are provided. The interrelated obstacles to more widespread use at present time are the cost and the quantity of the drug, but the initiated research studies promise a circumvention [15].
The randomized, multinational study, supported by the World Health Organization, to compare the efficacy and side effects of Mifepristone and two regimens of Levonorgestrel in Emergency contraception [10] will be a step forward in the research of emergency contraception methods. But some questions remain open about the mechanism of action of emergency contraception.
References
- P.F.A. Von Look and H. von Hertzen, "Emergency Contraception", British Medical Bulletin 49/1, 158-170, 1993.
- Anne Webb, "Emergency Contraception", Fertility Control Reviews 4/2:3-7, 1995.
- Paul F.A. Von Look and H. von Hertzen, "Clinical Uses of Antiprogestogens", Human Reproduction Updates 1/1:19-34, 1995.
- P.F.A. Von Look and H. von Hertzen, "Antiprogestogens: perspectives from a Global Research Program", 253-277, 1993.
- Helena von Hertzen and Paul F.A. Van Look, "Research on New Methods of Emergency Contraception", International Family Planning Perspectives 22/2:62-68, 1996.
- E. Kesserü et al., "The Normal and Peripheral Effects of d-Norgesterel in Postcoital Contraception", Contraception 10/4: 411- 424, 1974.
- World Health Organization, "Randomized Controlled Trial of Levonorgesterel versus the Yuzpe Regimen of Combined Oral Contraceptives for Emergency Contraception", The Lancet 352:428-433, 1998.
- Anna Glasier et al., "Mifepristone (RU 486) Compared with High-Dose Estrogen and Progestogen for Emergency Postcoital Contraception", The New England Journal of Medicine, 327:1041-1044, 1992.
- A Randomized Controled Trial Comparing Three Single Doses of Mifepristone in Emergency Contraception", to be published in The Lancet.
- Helena von Hertzen , "A Randomized, Multinational Study to Compare Mifepristone and two Regimes of Levonorgestrel in Emergency Contraception", UNDP/UNFPA/WHO/World Bank Special Programme of Research, Development and Research Training in Human Reproduction, Project 97902, 1997.
- Helena von Hertzen and Paul F.A. Van Look, "Alternative Methods of Emergency Contraception", Fertility Control Reviews 4/2:22-25, 1995.
- P.C. Ho and M.S.W. Kwan, "A prospective randomized comparison of Levonorgestrel with the Yuzpe regimen in post-coital contraception", Human Reproduction, vol.8 no.3, pp.389-392, 1995.
- Guillebaud J., " Time for emergency contraception with Levonorgestrel alone", Lancet 1998 Aug 8, 352(9126): 416-417.
- Sharon L. Camp, Ph.D., "Emergency Contraceptive Pills", Consortium for Emergency Contraception December 1996.
- Van Look, P.F., and Von Hertzen, H., "Post ovulatory methods for fertility regulation" Annual Technical Report 1992, Geneva World Health Organization 1993.
- "Consensus Statement on Emergency contraception", Conference on Emergency Contraception in Bellagio, Italy, April 1995.