Diaa M. El-Mowafi - Zagagig University, Egypt
Transvaginal Sonography and Hysteroscopy Versus Histopathology in Postmenopausal Bleeding
Diaa El-Mowafi MD, Ahmed Farid MD* and Ahmed El-Badawi MD**
Obstetrics and Gynecology, Radiology* and Pathology** Departments, Benha Faculty of Medicine, Eygpt
Abstract
Transvaginal sonography (TVS) and hysteroscopy were compared with the histopathological results of the dilatation and curettage (D&C) biopsies in 42 patients attending Benha University Hospitals with postmenopausal bleeding. Endometrial lesions were detected by histopathology in 23 cases (54.8%), 17 of them were diagnosed by TVS and 14 from the remaining 19 normal atrophic endometrium were diagnosed by it. This gave a sensitivity and specificity of 73.9% and 73.7% respectively and a predictive value as a positive test, as a negative test and efficacy of 77.3%, 70% and 73.8% respectively. This efficacy could be increased to 81% by taking into account 5 mm of endometrial thickness as a cut-off level between normal and abnormal endometrium with significant difference (P < 0.001). Hysteroscopy diagnosed 18 cases from the 23 endometrial lesions which had been diagnosed by histopathology and 16 from the remaining 19 normal atrophic endometrium. This gave a sensitivity and specificity of 78.3% and 84.2%, respectively and a predicative value as a positive test, as a negative test and efficacy of 85.7%, 76.2% and 81% respectively. This study shows that TVS allows detection of an endometrial pathology in the vast majority of cases and as it is easy, relatively cheap, needs no anaesthesia and non - invasive it can be used as the first diagnostic step in the investigations of women with postmenopausal bleeding to be supplemented, in the cases needed, by hysteroscopy and histopathological study of D&C biopsy. This will minimise cost, time and complications for the patient.
Introduction
Postmenopausal bleeding is a serious complaint as it is caused by a malignancy in 30 - 50% of cases in which there have been either continuous or repeated episodes of bleeding (Ross, 1988). Fractional curettage was always the ultimate investigation to exclude endometrial carcinoma and diagnose other pathology (Gusberg, 1988). This procedure has 2 main drawbacks : first it is an invasive one and has to be done under general anaesthesia, so it cannot be applied repeatedly in high risk patients and those with recurrent bleeding. Second it may miss lesions such as small polyps or small endometrial carcinoma in not less than 10% of cases (Renaer et al., 1983).
Thus, it would be valuable to develop other non - invasive methods for the early diagnosis of endometrial abnormalities, reducing the need for hospital curettage. Hysterosepy allows direct visualization of the uterine cavity without cervical dilatation and therefore, usually without anaesthesia, thus it could be used as an office technique in the evaluation of endometrial disorders (Gimpelson, 1992). More recently, transvaginal sonography (TVS) has permitted the use of higher frequency ultrasound at greater proximity to the uterus and the endometrial - myometrial interface can be seen clearly than with the full bladder transabdominal technique (Nasri et al., 1 99 1).
Measurement of endometrial thickness using TVS is helpful in diagnosis of endometrial pathology, including endometrial cancer (Grardbera et al.,1991) and in assessment of myometrial invasion (Cacciatore et al., 1994).
The present study was designed to compare prospectively TVS and hvsteroscopy findings in women with postmenopausal bleeding ,with the histopathological results of the D&C biopsy.
Subjects and Methods
Forty two patients attended the outpatient clinic in Benha University Hospitals with postmenopausal bleeding were included in this study. The mean age was 52.6 + 2.8 (sod.) years, range 48 - 58 years. The mean of postmenopausal period was 5.4 + 3.1 (s.d.) years, range 2-12 years. Ten patients were hypertensive, 5 had delayed menopause, 4 patients had received hormonal replacement therapy in the form of sequential oestrogen / progestogen, 2 patients were diabetic, 2 patients did not ever get pregnant before while the remaining patients had no obvious risk factor.
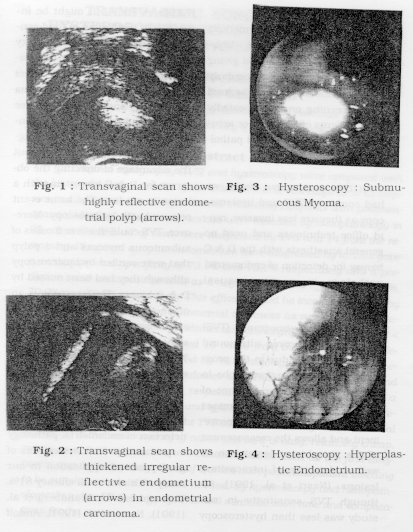
TVS was performed on admission by a transducer with an emission frequency of 5 MHz (Sono ACE- 4800 Medison - Korea). Detection of a hyperechoic area within the endometrial layers, was taken as suggestive of endometrial polyp (Fig. 1). Endometrial cancer was suspected when echoes were clearly dishomogeneous and the interface between the endometrium and myometrium was irregular, suggesting invasive growth (Fig. 2). Endometrial thickness was measured from the highly reflective interface of the junction of the endometrium and myometrium. This measurement represents the two layers of the endometrium.
Hysteroscopy was performed under general anaesthesia immediately before D&C by an operator unaware of TVS findings using (Karl Storz - Germany) hysteroscope, with a 5 mm diagnostic sheath. The uterine cavity was distended with CO2 using Hamou Microhyteroflator at pressure not exceeding 100 mmHg. Adequate visualisation of the uterine cavity was essential to admit the case in the study. All patients underwent D&C biopsy after hysteroscopy and sent for histopathological examination. Results were statistically analysed according to Steel and Torrie (1980) to detect the true positive (a), false negative (b), false positive (c) and true negative (d) results for endovaginal ultrasound and hysteroscopy versus the histopathological report of the D&C biopsy. Sensitivity of the tool was calculated as a / a + b x 100, specificity = d / d + c x 100, predictive value as a + ve test = a / a + c x 100, predictive value as a -ve test d / d + b x 100 and efficacy = a + d / a + b + c + d x 100.
Results
The histopathological diagnosis of our 42 cases showed normal postmenopausal atrophic endometrium in 19 cases (45.2%), chronic endocervicitis was diagnosed in 5 of them. An endometrial pathology was found in 23 patients (54.8%): endometrial hyperplasia was diagnosed in 8 cases (19%), a polyp was found in 11 cases (26.2%), endometritis was found in 2 cases (4.8%) and endometrial carcinoma was the histopathological report of 2 cases (4.8%). Endometrial echoes were visualised and measured by TVS in all cases. An abnormal endometrial texture was found in 17 of the 23 cases with endometrial pathology (sensitivity 73.9%). Hyperplasia was diagnosed in 7 of the 8 cases, while the other case was diagnosed as normal atrophic endometrium. A polyp was diagnosed in 9 cases of the 11, while the other 2 cases were diagnosed as normal atrophic endometrium. The 2 cases of endometritis were diagnosed by TVS as hyperplasia.
From the 2 cases of endometrial carcinoma one case was correctly diagnosed by TVS (Fig. 2) while the other was diagnosed as a polyp due to absence of invasion. Submucous myoma were diagnosd by 'IVS and had been verified by hysteroscopy in 2 cases (Fig. 3) who had been missed by D&C histopathological examination and atrophic endometrium was obtained only. Also three cases from the atrophic endometrium were diagnosed by TVS as polyps but only one of them was verified by hysteroscopy. Thus the specificity of 'TVS was 73.7%, its predictive value as a positive test was 77.3%, its predictive value as a negative test was 70.0% and its overall efficacy was 73.8%.
Hysteroscopy had diagnosed 18 cases from the 23 lesions that had been diagnosed by histopathology (sensitivity 78.3%). Hyperlpasia was diagnosed in 6 of the 8 cases (Fig. 4), while the other 2 cases were diagnosed as normal atrophic endometrium and endometritis. A polyp was diagnosed in 10 of the 11 cases while the other case was diagnosed as polypoidal hyperplasia. One of the 2 cases of endometritis was diagnosed correctly while the other was diagnosed as hyperplasia . One of the 2 cases of endometrial carcinoma was diagnosed correctly by hysteroscopy while the other case was diagnosed as polypoidal hyperplasia. Thus the specificity of hysteroscopy was 84.2%, its predictive value as a positive test was 85.7%, its predictive value as a negative test was 76.2% and its overall efficacy was 81%.
The endometrial thickness was significantly lower (P < 0.001) among patients with normal atrophic endometrium than in other lesions (Table 3). Five mm endometrial thickness was taken as a cut line below which the endometrium was considered normal atrophic and if it is equal or more than 5 mm, endometrial lesion is expected. This cut line gave a false negative results in 3 cases and a false positive results in 5 cases. This rule had a sensitivity of 87%, specificity of 73.7%, predictive value as a positive test 80%, predictive value as a negative test 82.4% and an overall efficacy 81%.
Table 1 : Findings in the studied group by the 3 different methods.
Histopathology |
TVS |
Hysteroscopy |
| Normal atrophy (N = 19) | Atrophy (14) | Atrophy (1 6) |
| Polyp (3) | Polyp (1) | |
| Myoma (2) | Myoma (2) | |
| Hyperplasia (N = 8) | Hyperplasia (7) | Hyperplasia (6) |
| Atrophy (1) | Atrophy (1) | |
| Endometritis (1) | ||
| Polyp (N = 11) | Polyp (9) | Polyp (10) |
| Atrophy (2) | Hyperplasia (1) | |
| Endometritis (N = 2) | Hyperplasia (2) | Endometritis (1) |
| Hyperplasia (1) | ||
| Carcinoma (N = 2) | Carcinoma (1) | Carcinoma (1) |
| Polyp (1) | Hyperplasia (1) |
N = number of patients.
Table 2 : Statistical analysis of the findings in TVS and hysteroscopy versus histopathology.
TVS |
Hysteroscopy |
|
| True + ve (a) | n = 17 |
n = 18 |
| False - ve (b) | n = 6 |
n 5 |
| False + ve (c) | n = 5 |
n 3 |
| True - ve (d) | n = 14 |
n = 16 |
| Sensitivity | 73.9% |
78.3% |
| Speciticity | 73.7% |
84.2% |
| Predictive + ve | 77.3% |
85.7% |
| Predictive - ve | 70.0% |
76.2% |
| Efficacy | 73.8% |
61% |
Table 3 : Endometrial thickness measured by TVS in relation to histopathological findings.
| Hysteroscopy | TVS Endometrial thickness |
| Atrophy | 3.8 ± 1.8 (2 - 6) |
| Hyperplasia | 12.9 + 7.2 (4 - 26) |
| Endometritis | 12.5 ± 0.7 (12.13) |
| Polyp | 15.3± 7.9 (2.29) |
| Carcinoma | 21.1 + 9.8 (12 - 30) |
Table 4 : Statistical analysis of the endometrial thickness measured by TVS versus histopathology.
TVS |
|
| True + ve (a) | n = 20 |
| Faise - ve (b) | n = 3 |
| False + ve (c) | n = 5 |
| True - ve (b) | n = 14 |
| Sensitivity | 87% |
| Specificity | 73.7% |
| Predictive + ve | 80% |
| Predictive - ve | 82.4% |
| Efficacy | 81% |
Discussion
The ideal diagnostic method should be safe, less or non-invasive, less costly, simple and giving a rapid result. This is particularly needed if this method will be used as a screening one or repeatedly as in patients of high risk or actually developed endometrial pathology.
In this prospective study, we had compared TVS and hysteroscopy as they are less invasive, rapid office techniques and need no general anaesthesia with the D&C biopsy for detection of endometrial pathology in postmenopausal bleeding.
Transvaginal sonography ('IVS) has greatly improved ultrasound image resolution due to the proximity of the endovaginal probe to the endomtrium. The absence of the full bladder which compresses the uterus enhances this improvement and allows the measurement of the atrophic endometrium as well as detection of intracavitaly lesions. (Nasri et al. 1991). Although TVS sensitivity in our study was less than hysteroscopy (73.9% vs 78.34), it might be increased by instillation of fluid contrast into the uterine cavity (Fedele et al., 1991, Syrup and Sahakian, 1992). 'IVS could detect one case of endometrial carcinoma in our study and as the other case was polypoidal growth of the cancer without invasion it was diagnosed as an endometrial polyp but the advantage of directing the observer for D&C biopsy in such a lesion is not lost. The same event occurred with hysteroscopy. Moreover, 'IVS could discover 2 cases of submucous myomas and a polyp that were verified by hysteroscopy although they had been missed by D&C biopsy. Hysteroscopy is an office technique which allows in expert hands, a direct and reliable visualisation of the uterine cavity. This may explain its higher overall efficacy than TVS in our study.
Taking 5 mm endometrial thickness as a cut-off level for detection of endometrial pathology in postmenopausal women was of good practical application in our study with an overall efficacy 81%. This agrees with Grandberg et al. (1991), Nasri et al. (1991), Andolf et al. (1993) and Cacciatore et al. (1994). Our results although less but near to that reported by Cacciatore et al. (1994). For TVS the sensitivity and specificity versus endometrial pathology were 73.9% and 73.7% respectively while in Cacciatore et al. (1994) study they were 73.9% and 95.7%. For hysteroscopy. The sensitivity and specificity versus endometrial pathology were 78.3% and 84.2% respectively while in Cacciatore et al. (1994) study they were 86.9% and 91.7%. This difference honestly can be attributed to more experience which is an important factor in these tools of investigations. Ultimately the diagnostic accuracy of TVS and hysteroscopy depends on the experience and skill of the operator. This study shows that, although less sensitive than hysteroscopy for the direct diagnosis of endometrial pathology,TVS can reach a higher sensitivity once endometrial thickness is taken into account. In addition, the presence of myometrial invasion of endometrial cancer and detection of other possible concomitant pelvic pathology can be reached during TVS (Goldstein, 1994). Since TVS is relatively cheap, easy, needs no anaesthesia and non-invasive, it could be used as a first choice diagnostic test in the investigation of women with postmenopausal bleeding. TVS can select those cases in which the likelihood of endometrial pathology is high i.e. when the endometrial thickness is 5 mm or more. In these cases D&C biopsy integrated by hysteroscopy should be used for achieving a proper diagnosis.
References
- Andolf E., Dahlander K. and Aspenberg P. (1993): Ultrasonic thickness of the endometrium correlated to body weight in asymptomatic postmenopausal women. Obstet. Gynecol. 28 : 936 - 940.
- Cacciatore B., Ramsoy T., Lehtoirta P. and Ylostalo P. (1994) : Transvaginal sonography and hysteroscopy in postmenopausal bleeding. Acta Obstet. Gynecol. Scand, 73 : 413 - 416.
- Fedele L., Bianchi S., Dorta M. and Brioschi D. (1991): Transvaginal ultrasonography versus hysteroscopy in the diagnosis of uterine submucous myoma. Obstet Gynecol. 77: 745 - 748.
- Gimpelson R. (1992) : Office hysteroscopy. Clin. Obstet. Gynecol. 35: 270 - 281.
- Goldstein S. (1994) : Use of ultrasonohysterography for diagnosis of perimenopausal patients with unexplained uterine bleeding. Am. J. Obstet. Gynecol 170: 565 570.
- Grandberg S., Wickland M., and Karlsson B. (1991) : Endometrial thickness as measured by endovaginal ultrasound for identifying endometrial abnormalties. Am. J. Obstet. Gynecol. 164 : 47 52.
- Gusberg S. (1988) : Diagnosis and principles of treatment of cancer of the endometrium. In: Females Genital Cancer, Eds. G Deppe, Chirchill Living Stone, New York, pp 337 - 360.
- Renaer M., Vandervoort L., Ide P. and De Wolf F. (1983) : Investigation of patients with postmenopausal bleeding. In : Hysteroscopy. Ed. Van der Pas H. et al., MTP Press Limited, Boston, USA 121-128.
- Ross L. (1988) : Pelvic Ultrasound - should it be used routinely in the diagnosis and treatment of postmenopausal bleeding? J. Royal Soc. Med. 81 723 - 724.
- Steel R. and Torrie G. (1980) Principles and Procedures of Statistics. Ed. Me Graw - Hill, P - P, 40 - 45.
- Syrup C. and Sahakian V. (1992) : Transvaginal sonographic detection of endometrial polyps with fluid contrast augmentation. Obstet. Gynecol. 79 : 1041-1043.