Postgraduate Training Course in Reproductive Health/Chronic Disease
Community-based Intervention
for Prevention and Control of Cardiovascular Diseases
Dongbo Fu
Department of Preventive Medicine, School of Public Health, Fudan University, Shanghai, China
Tutors
Ruitai Shao
National And Community Programmes Noncommunicable Disease Prevention and Health Promotion
World Health Organization
Mark van Ommeren
Department of Mental Health and Substance Dependence, World Health Organization
See also ![]() presentation
presentation
Introduction
Cardiovascular diseases (mainly ischaemic heart disease and stroke) has been the leading cause of death worldwide.The majority of all deaths attributable to cardiovascular dieases (CVDs) are in developing countries.There is now a pressing need for developing countries to define and implement preventive interventions for CVDs. 1
In the early 1950s, CVDs were already an important health issue in developed countries. On the basis of accumulated scientific evidence from epidemiological studies and research on preventive medicine showing that cardiovascular diseases are associated with unhealthy lifestyles and human behaviours, the concept of community intervention was introduced to the field of cardiovascular disease prevention in the late 1960s and early 1970s in developed countries2. Major community-based cardiovascular disease prevention programs have been conducted in North Karelia, Finland; the state of Minnesota; Pawtucket, Rhode Island; and in three communities and in five cities near Stanford,California, USA. Those community-based CVD prevention programs were soon followed by several other projects of the same kind, in Europe, Israel, South Africa. A number of projects are also being carried out as demonstration projects of WHO-related programmes: CINDI (by the WHO Regional Office for Europe(EURO)), CARMEN (by the WHO Regional Office for the Americas (AMRO)), and Interhealth (WHO headquarter) 2,3. In conjunction with the WHO Interhealth Programme, which was started in 1986, many developing countries have been invloved in the similar activities of community-based CVD prevention and control3.
The mortality of cardiovascular diseases is decreasing in developed countries as a result of long-term promotion of healthy lifestyles and community prevention measures. However, with ageing populations and rapidly changing lifestyles (in particular, tobacco smoking, unhealthy diets, and physical inactivity), the
burden of CVDs is increasing in almost all developing countries4. The evidence-based, affordable approaches for CVD prevention and control are needed, especially in low- and medium-resource settings in developing countries. The successful experiences and scientific evidence for CVD prevetion and control achieved in the past 30 years in developed countries make it possible for the developing countries to find the appropriate approaches to address CVDs.
Objectives
The objectives of this paper is to identify evidence-based, cost-effective community-based strategies and intervetions for CVD prevention and control;and to form recommendations for the appropriate use of the community-based interventions in the developing countries.
Methods
This paper was a literature review.
Criteria for considering studies for this review
A community-based intervention for cardiovascular disease prevention and control is defined as any primary prevention and secodary prevetion program that attempted to reduce the population burden of CVDs by modifying at least one cardiovascular risk factor (ie. blood pressure, smoking, total blood cholesterol, physical activity, diet) and providing health services in the community. Intervention studies meeting this definition were included in this review.
Search strategy for identification of studies
MEDLINE 1966 to March 2003 using medical subject heading “community”, “intervention*”, “cardiovascular disease*” together with relevant diagnostic terms(ie. coronary heart disease and stroke)and text word searches for specific interventions(see below). Searches of reference list of papers, and also use hand searching.
- community
- intervention*
- prevention*
- control
- cardiovascular disease*
- coronary heart disease
- stroke
1 and (2 or 3 or 4) and (5 or 6 or 7)
limit to “title/abstract”.
- quality of life
1 and (2 or 3 or 4) and (5 or 6 or 7) and 8
limit to “title/abstract”.
Findings
According to the commonly used classification of prevention5, the studies included in this review were divided into two main types: community-based primary prevention and community-based secondary prevention. The community-based primary prevention was classified to more subgroups concerning different criteria.
1.Community-based interventions for primary prevention of CVD
Since the early 1970s, most of the intervention programs for cardiovascular disease conducted in the communities were belong to primary prevention, aiming to reduce the cardiovascular risk factors and reduce morbidity and mortality from cardiovascular disease in whole communities. Those programs differ in their settings(rural or urban community, developed or developing country), methods, components and intensity of the interventions, in the risk factors targets, and in the evaluation measurements, periods, designs and effects. Concerning different ways, those community-based intervention programs can be divided into several different classifications:
(1) According to perspectives to prevention, they can be classified as High-Risk Approach versus Population Approach.
The traditional epidemiological studies of determinants of cardiovascular disease offers the opportunity to target those individuals who are likely to develop CVD and those most likely to benefit from prevention and treatment efforts and, thus, could play a role in preventing and control CVD. The results of the programs using high-risk approach(sometime call it individual approach) proved that they were efficient to reduce incidence of CVD among the high risk individuals even in less than five years. One example is a study from China6. In the study in 1987 in 7 cities, a cohort containing about 2700 subjects(35 yeas and over) free of stroke was sampled in each community. Screening was administered to the cohort in the intervention communities for the eligible subjects(hypertension, heart disease, and diabetes) for intervention. A program of treatment for those subjects was instituted in the intervention cohort----“every week doctors from collaborating center hospitals and primary prevention branches went to the local health stations to see study patients”. Although the intervention included health education to the full intervention community, but the result only showed the follow-up of the cohort. The result demonstrated that the 3.5-years cumulative incidence of total stroke was significantly lower in the intervention cohort than the control cohort (0.93% versus 1.34%; RR=0.69; 95%CI, 0.57 to 0.84).
Most major large-scale community-based cardiovascular disease intervention projects use population approach or combination of high-risk approach and population approach ---- “comprehensive community-based approach” 7-21. They all use a quasi-experimental design. They all carry out comprehensive interventions activities, involving innovative media campaigns, local media, community participation, co-operation with local and
national sectors and policy making. They all carefully planned. Their intervention activities and process are based on sound theoretical frameworks (such as community organization, social learning theory, social marketing, ecological health promotion model). They all use independent cross-sectional randomized sample of the community to compare the net change of the targeted risk factors. And also compare the trend of the risk factors and CVD morbidity and mortality rates in the intervention communities and reference communities. They usually show a modest effect on the target risk factors or disease rates depending on the intensity of the intervention in each project2, 22. The representatives of those major projects included several very famous first and second generation community-based heart health intervention projects both in the Europe and in the USA: the North Karelia Project (Finland), the Stanford Three-Community Study (USA), Stanford Five-City Project (USA), Minnesota Heart Health Program (USA), the Swiss National Research Programme, the German Cardiovascular Prevention Study, and the Kilkenny Health Project (Ireland). Among them, North Karelia Project is the most successful one, which first conducted as demonstration programme, after the original project period, their experience has actively been applied for national action2,3. And as the first major community-based project for CVD prevention, North Karelia project was soon followed by several other project of the same kind both on national level and global level. For example, it led to demonstration projects of WHO-related programmes: Comprehensive Cardiovascular Community Control Program (CCCCP)(by WHO/the WHO Regional Office for Europe(EURO)) CINDI (by EURO), CARMEN (by the WHO Regional Office for the Americas(AMRO)), and Interhealth (WHO headquarter). In conjunction with the WHO Interhealth Programme, which was started in 1986, many developing countries have been involved
in the similar activities of community-based CVD prevention and control2. Of course, those projects use population approach or high-risk approach and population approach in combination.
(2) According to how many risk factors targets, the programs can be classified as Single Cardiovascular Risk-Management versus Comprehensive Cardiovascular Risk-Management.
CVD prevention too frequently focuses on single risk factors rather than on comprehensive cardiovascular risk23. There were many prevention programs only addressed one risk factors of CVD to test the effect of the targeted risk factor change or its impact on CVD incidence, morbidity or mortality, such as high blood pressure control, cholesterol concentration reduction, changes in nutrition, community-based smoking cessation23-27. Although single cardiovascular risk-management approach can be effective, many intervention studies demonstrated that for CVD prevention activities to achieve the greatest benefits, a paradigm shift is required from the treatment of risk factors in isolation to a comprehensive cardiovascular risk-management approach28. Why we should focus on integrated multifactorial approach in community primary prevention for CVD is also because two or more cardiovascular risk factors clustering in one person is very common in the real life, and the clustering of risk factors may act synergistically increasing the risk more than any one single factor acting alone23,29. Majority of the major community-based intervention projects, who use population approach also deal with more than one “classical” risk factors at the same time, and emphasized both diet and smoking.
(3) According to the components of interventions, the programs can be classified as Individual behavior Change (educational approach) versus Policy and Environmental changes.
Community-based CVD prevention projects in the USA, such as Stanford Three-Community Study, Stanford Five-City Project, Minnesota Heart Health Program, Pawtucket Heart Health Program, Community Intervention for Smoking Cessation (COMMIT), are the representatives of individual behavior change approach user24. Those projects recognize the multifactorial nature of cardiovascular disease and consistently advocate approaches involving multiple strategies across multiple channels and across all sectors of the population. However, their main focus has been on interventions to encourage individual behavior change, on information and skill building. Environmental and policy approaches have not received much attention in the projects in the United States. Since the limited perspectives, the projects could not achieve the greatest impact comparison of the projects used policy and environmental approaches. For example, in Stanford Five-City Project, the intervention conducted in the treatment cities was a 6-year multifactor risk reduction program including newspapers, television and radio, mass-distributed print media, classes, contents, and correspondence courses10. The results showed that changes in risk factors were observed, but no evidence of a treatment-control difference in terms of combined-event rate of cardiovascular disease between 1979 and 19929,22.
On the contrary, community-based projects to prevent cardiovascular disease in the Europe, who using approaches focusing on policy and environmental changes have been more successful than those in the USA. Finland’s North Karelia Projects is a classic example of a comprehensive public health program to prevent cardiovascular disease that incorporates policy and environmental interventions in an effective,
community focused manner. The results indicated that major changes have taken place in the levels of target risk factors in North Karelia (Table 1) 3. By 1995 the annual mortality rate of coronary heart disease in the middle age (35-64years) male population in North Karelia has reduced about 73% form the pre-program years(Graphic 1) 3,11. The risk factors targeted by the program could explain most of the decline in ischamic heart disease observed over 20 years30. Another example is Heartbeat Wales project. The important strategy of the project was “ to achieve environmental, organizational, structural, and policy changes to support healthy choices by individuals” 31.
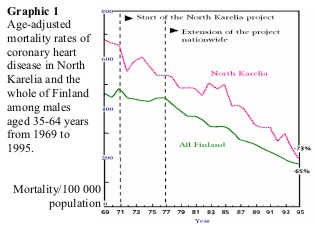
Table 1. Risk facotor changes in North Karelia 1972-1997(30-59Years)
| Men | Women | |||||
| Year | Smoking % | S-Cholesterol mmol/l | Blood Pressure mmHg | Smoking % | S-Cholesterol mmol/l | Blood Pressure mmHg |
| 1972 | 52 | 6.9 | 149/92 | 10 | 6.8 | 153/92 |
| 1977 | 44 | 6.5 | 143/89 | 10 | 6.4 | 141/86 |
| 1982 | 36 | 6.3 | 145/87 | 15 | 6.1 | 141/85 |
| 1987 | 36 | 6.3 | 144/88 | 16 | 6.0 | 139/83 |
| 1992 | 32 | 5.9 | 142/85 | 17 | 5.6 | 135/80 |
| 1997 | 31 | 5.7 | 140/88 | 16 | 5.6 | 133/80 |
(4) Intervention characteristics of the successful community-based primary prevention programs for CVD prevention and control
Some common intervention and design characteristics can be identified through summary all of the large-scale comprehensive community-based cardiovascular disease prevention and control projects (especially North Karelia project):
---carefully planned using sound health promotion model
---interventions and process are based on scientific theories and frameworks.
--comprehensive intervention approach: combination of population approach and high-risk approach; Multi-components including: mass communication, specific health education, community organization, policy and environmental change, co-operation with the other sectors.
---focusing on policy and environmental change intervention strategies and community diagnosis, community organization and participation.
---quasi-experimental design, long time follow-up and proper evaluation.
2. Community-based Interventions for secondary prevention of CVD
The effective community-based secondary prevention programme would prevent many deaths that occur in middle- and older age and substantially reduce disability related to CVD. 32
(1) Evidence base
Patients with established CVD constitute one of the highest risk groups. Secondary prevention involves identifying, treating and rehabilitating these patients to reduce their risk of recurrence, to decrease their need for interventional procedures, to improve their quality of life and to extend their overall survival32. Several studies have demonstrated the effective-ness of community-based secondary prevention interventions in the control of CVDs33-35. From the early1980s the WHO-MONICA study monitored trends in coronary heart disease over 10 years, across 38 populations, in 21 countries. Data from this study indicate that secondary prevention and changes in coronary care are strongly linked with declining coronary end-points. It is now clearly evident that lifestyle changes such as smoking cessation, healthy dietary practices, weight control and regular moderate physical activity, can significantly contribute to reduction in cardiovascular mortality in people with established CVD and their recurrence.
(2) Indicators of quality of life for CVD patients
As mentioned above, quality of life should be a key objective of interventions for patients with CVD, not only to prevent or to retard the progression of the underlying disease but also to alleviate symptoms and to improve the patients’ functional capabilities. However, few community-based interventions for patients with CVD address their impacts on patients’ quality of life. One reason is that a sensitive and valid tool for assessment of quality of life for CVD patients may not be available. Lack of assessment instruments makes it difficult for health service providers to identify the needs of patients, and less fitted interventions or services provide. Here I will briefly describe existing quality of life assessment tool and indicators for testing effectiveness of CVD interventions or treatments.
There is no consensus definition of quality of life until now. Quality of life has been defined by WHO as “individuals’ perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards and concerns”36. Different quality of life assessment tools are based on different concepts and consist of different domains (dimensions) of quality of life. The WHOQOL instruments (the WHOQOL-100 and the WHOQOL-BREF) are based on the quality of life concept just described and have six domains36. These are: (a) physical domain; (b) psychological domain; (c) level of independence; (d) social relationships; (e) environment; and (f) spirituality/religion/personal beliefs. There are twenty-four facets (subdomains) are incorporated within six domains. Quality of life assessment instruments can be classified as (a) generic instruments to assess quality of life in a variety of situations and population groups and (b) specific instruments to assess quality of life of specific populations (e.g. cancer patients, the
elderly).
Table 2. Summary of commonly used questionnaires and indicators for assessment of quality of life in patients with CVD
| Dimension | Measures |
| Psychological | |
| Global emotional | Supplemented Nottingham Health Profile |
| Anxiety | State-Trait Anxiety Inventory |
| Depression | Center for Epidemiologic Studies-Depression Scale |
| Neuropsychological | Neuropsychological measures |
| Social interactions | |
| Family | Supplemented Nottingham Health Profile |
| Nonfamilial | 3-item social activity scale |
| Symptom relief | |
| General symptom relief | Health status index Supplemented Nottingham Health Profile |
| Pain (Angina and related) | Cardiac-related symptoms and specific activities scale |
| Functional capacity and role activities | |
| General functioning | Standardized physical functional Status measures (e.g. ADL) |
| Vocational functioning | Standardized adjusted to illness scale |
| Avocational functioning | SF-12 |
| Sexual functioning | Interview The sexual symptom distress index |
| Economic | |
| Return to work/ Personal productivity | Self-report |
| Cost-effectiveness | Hospital costs, length of hospital stay |
| Individual economic impact | Self report, financial status |
| Life satisfaction | General health questionnaire |
| Perceptions of general health status or well-being | GHQ, The psychological general well-being(PGWB) |
| Sleep disturbance | The sleep dysfunction scale |
| Side effects | Minor symptom evaluation profile Subjective symptom-Assessment profile |
The aforementioned WHOQOL instruments, for instance, are generic ones, which have six uses: in medical practice; improving the doctor-patient relationship; in assessing the effectiveness and relative merits of different treatments; in health services evaluation; in research; and in policy making. Although many studies on quality of life in patients with CVD can be found33,37, no specific instrument exists. Normally different scales are used together to assess the quality of life in patients with CVD according to different concepts and narrow or broad domains covered.
In terms of quality of life assessment for testing effectiveness of CVD interventions, the studies and practices have been predominantly done in clinical settings, including assessment of changes in quality of life for patients receiving coronary artery bypass grafting (CABG), percutaneous tansluminal coronary angioplasty (PTCA), cardiac transplants, valvular surgeries, exercise rehabilitation, and so on37 The commonly used questionnaires (scales), domains (Indicators) are listed in Table 2.
Discussion
CVD Prevention at the community-level is essential because modifiable causal risk factors are deeply entrenched in the social and cultural framework of society. From the limited publications included in this paper, several experiences and evidence should be completely understood and emphasized.
1. Both community-based primary prevention and secondary prevention are needed for CVD prevention and control
Primary intervention is directed to susceptiable people before they develop a cardiovascular disease. The key objective of primary prevention is to reduce the incidence of disease and consequently, its sequelae5. But the effects of CVD prevention and control must include not only changes in the frequency and severity of CVDs but also preventing recurrence of the established CVD, reducing mortality of those patients and improving their quality of life. The World Health Organization global strategy for the prevention and control of noncommunicable disease emphsized that in addition to reducing the common risk factors in the population, secondary prevention of major cardiovascular events (fatal and non-fatal myocardial infarction; fatal and non-fatal stroke; sudden cardiac death, re-vascularization procedures) should be regarded as a key component of any public health strategy to reduce the rising burden of CVD in low and middle income countries32. But we should avoid completely using less cost-effective secondary interventions, such as high-tech methods to identifying patients, pharmacological methods to treat patients. The key areas for improving secondary prevention of major CVD include: community-based approach, patient-oriented delivery system and support for self-management32.
2. Community-based primary prevention of CVD should target main cardiovascular risk factors, especially four behavioral risk factors(tobacco, unhealthy diet, physical inactivity, alcohol) using comprehensive risk-management strategies
World Health Report 2002 showed that, obesity, high blood pressure, high cholesterol, alcohol and tobacco – independently and often in combination, are the major causes of CVDs38. The scientific evidence is strong that a change in dietary habits, physical activity, tobacco control and alcohol consumption can produce rapid changes in population risk factors for CVDs. Comprehensive risk-management for community cardiovascular risk decreasing is because CVD is multifactorial disease process39. Many people have more than two cardiovascular risk factors at the same time.
3. Community-based primary prevention of CVD need combination of population approach and high-risk approach
Cardiovascular risks often occur as a continuum throughout the population. Shifting population distributions of exposure can gain large potential reduction in CVD morbidity and mortality39. Since most CVD occurs in the masses of people not at the highest risk level(high-normal to borderline level), high-risk approach will do little to quell the current epidemic of CVD, especially in the developing countries, where limited medical resources can not afford the interventions mainly relying on treatment of high risk subjects. For example, a high-risk approach can only target 25% of the community population with elevated blood pressure23. A combination of high-risk and population-based approach is essential to shift the cardiovascular risk profile. Prevention through population-wide behavior modification will be more cost effective than high-risk approach intervention39. The changes in risk achieved in population-based studies are often small, but it should be realized that even small changes in the distribution of risk factors in the population will bring about sizable changes in CVD mortality as demonstrated among different countries. For instance, for every 1% decrease in the serum cholesterol level there is an associated 2% reduction in coronary heart disease(CHD) rates39.
Furthermore, high-risk intervention should more focus on routine health counseling in primary health system and other evidence-based, cost-effective measures which have the feasibility of being implemented on a mass scale.
4. A major emphasis and strength of the community interventions for CVD prevention and control should be attempted to change social and physical environments in the community
Behavioral psychologist have long recognized that behavior change may not depend on personal factors, but be more influenced by the social and physical environmental elements, especially for behaviors like physical activities, eating habits, stop smoking, which need to maintain day after day. Since a change in environmental or policy is taken on the societal level to reduce exposure to health risks or to lead to healthy behavior, and do not require individuals to take action, it is more likely to be successful than individual change efforts to promote and maintain individual’s behavior change. Another rationale for expanding community-based programs to include more environmental- and policy-level activities comes from behavioral science theory(e.g., the theory of diffusion of innovations) 39. Individual-centered efforts are appropriate for the “early adopters” in the community to make positive health choices based mainly on new information. As for more “later adopters” in the community, we need the programs focusing more on health-fostering policies and environments.
5. Using life course perspective to consider community cardiovascular disease prevention and control
Most of community intervention programs are limited to the community resident aged 25 years and over. The risk of CVD is influenced by social and biological exposures not only in adulthood but also in fetal life, infancy, childhood, adolescence. Some studies confirmed the origin of atherosclerosis in childhood and showed that the prevalence and extent of fatty streaks and fibrous plaques increase rapidly during the 15- to 34-year age span39.
The life course perspective carries the potential of identifying the most appropriate and effective prevention strategies in different populations, because it considers the factors and processes that act at all stages of the life-span to affect risk of later disease40. Since the earlier in the CVD process preventive measures are instituted, the greater the likelihood for overall effectiveness and benefit, more community-based primary prevention programs target the youth aged less than 18 years should be advocated in the future.
6. Improving quality of life in patients with CVD
Future community-based intervention for CVD prevention and control, especially secondary and tertiary prevention, should pay more attention to improve the quality of life in patients with CVD and related high-risk populations. The measurement of quality of life should include developing new specific instruments or identifying more suitable questionnaires both multi-dimensional ones (e.g. the WHOQOL instruments ) and scales for one specific dimension.
Conclusion and recommendations
Although not including all related publications, this review clearly show that there are strong evidence base for community-based intervention for CVD prevention and control. The success of community-based intervention for CVD prevention and control achieved in the past 30 years and experience of a few similar projects in developing countries, provide the ideas, approaches, strategies, models to help the developing countries and low-resource developed countries to address CVD.
In all, as the WHO advocate: we now have the required base of science and technology to effectively reduce the public health impact of CVD. Let us “use what we know”. However, the following recommendations for implementation of community-based interventions for CVD prevention and control should be considered.
- adapting rather than adopting or copying the existing knowledge and experience in developed countries because each community is unique. Community assessment (community diagnosis) should be included in the first phase of a community intervention program for CVD prevention and control
- carefully planning of the program with a good understanding the community, sound theories, frameworks and health promotion models
- the community-based CVD intervention program should emphasize on comprehensive approaches, integrated risk management, policy and environmental changes, community organization, individual empowerment and participation, collaboration with various sectors
- scientific design and proper evaluation
- the program should be not only a demonstration programme to explore the best implementation model in the specific setting but also be expand to national actions
Reference
1. Razum O, Borchert M, Scheuermann W. Editorial: Do We Need Population Monitoring Laboratories to Evaluate Community-based Prevention of Cardiovascular Disease in Developing Countries? Tropical Medcine and International Health. 1998, 3(4):251-255.
2. Nissinen A, Berrios X, Puska P. Community-based Noncommunicable Disease Interventions: lesions from developed countries for developing ones. Bulletin of the World Health Organization. 2001,79:963-970.
3. Puska P. Successful Prevention of Non-communicable Diseases: 25 year experiences with North Karelia Project in Finland. Public Health Medicine.2002; 4(1):5-7.
4. Ebrahsim, S, Davey Smith, G. Exporting failure? Coronary Heart Disease and Stroke in Developing Counties. International Epidemiologcial Association. 2001, 30: 201-205.
5. Brownson RC., Remington PL., Davis JR. Chronic Disease Epidemiology And Control(Second Edition). American Public Health Association. 1998.
6. Fang XH, Kronmal R.A, Li SC, Longstreth W.T., Cheng XM, Wang WZ, et al. Prevention of Stroke in Urban China A Community-Based Intervention Trial. Stoke.1999;30:495-501.
7. Shea S, Basch CE. A review of five major community-based cardiovascular disease prevention programs. Part I: Rationale, design, and theoretical framework. American Journal of Health Promotion.1990,4(3):203-213.
8. Luepker RV, Murray DM, Jacobs DR, Mittelmark MB, Bracht N, Carlaw R, et al. Community Education for Cardiovascular Disease Prevention: Risk Factor Changes in the Minnesota Heart Health Program. American Journal of Public Health 1994;84(9):1383-1393.
9. Fortmann SP., Flora JA., Winkleby MA., Schooler C, Baylor C.B, Farquhar JW. Community Intervention Trials: Reflections on the Stanford Five-City Project Experience. American Journal of Epidemiology. 1995, 142(6): 576-587.
10. Winkleby MA., Feldman HA., Murray DM. Joint Analysis of Three U.S. Community Intervention Trials for Reduction of Cardiovascular Disease Risk. J Clin Epidemiol. 1997,
50(6):645-658.
11. Puska P, Vartiainen E., Tuomilehto J., Salomaa V., Nissinen A. Changes in Premature Deaths in Finland: Successful Long-term Prevention of Cardiovascular Diseases. Bulletin of the World Health Organization. 1998, 76(4):419-425.
12. Muntoni S, Stabilini L, Stabilini M, Muntoni S. Result of a Five-year Community-based Programme for Cardiovascular Disease Prevention: The ATS-Sardegna Campaign. European Journal of Epidemiology. 1999, 15: 29-34.
13. Weinehall L, Westman G, Hellsten G, Boman k, Hallmans G, Pearson TA, et al. Shifting the Distribution of Risk: Results of a Community Intervention in a Swedish Programme for the Prevention of Cardiovascular Disease. J Epidemiol Community Health 1999, 53: 243-250.
14. Vartiainen E, Jousilahti P, Alfthan G, Sundvall J, Pietinen P, Puska P. Cardiovascular risk factor changes in Finland, 1972-1997. International Epidemiological Association. 2000, 29: 49-56.
15. Scheuermann W., Razum O., Scheidt R., Wiesemann A., Frankenberg H.V, Topf G., et al. Effectiveness of a decentralized, community-related approach to reduce cardiovascular disease risk factor levels in Germany. The European Society of Cardiology. 2000,21, 1591-1597.
16. Fortmann SP., Varady AN. Effect of a Community-wide Health Education Program on Cardiovascular Disease Morbidity and Mortality. American Journal of Epidemiology. 2000, 152(4): 316-323.
17. Pekka P, Pirjo P, Ulla U. Influencing public nutrition for non-communicable disease prevention: from community intervention to national programme--experiences from Finland. Public Health Nutr 2002,5(1A):245-51
18. Soweid RA, Nakkash R, Nehlawi M, Khogali M. Together for Heart Health: An initiative for Community-based Cardiovascular disease Risk Factor Prevention and Control. Beirut, Lebanon September 1998-March 2002.
19. Osler M, Jespersen NB. The Effect of a Community-based Cardiovascular Disease Prevention Project in a Danish Municipality. Dan Med Bull. 1993, 40: 485-489.
20. Alcalay R, Alvarado M, Balcazar H, Newman E, Huerta E. SALUD PARA SU CORAZON: A Community-based Latino Cardiovascular Disease Prevention and Outreach Model. Journal of Community Health. 1999, 24(5):359-378.
21. Shea S, Basch CE. A review of five major community-based cardiovascular disease prevention programs. Part II: Intervention strategies, evaluation methods, and results. American Journal of Health Promotion.1990,4(4):279-87.
22. Sellers DE., Crawford SL., Bullock K, Mckilay JB. Understanding the Variability in the Effectiveness of Community Heart Health Programs: a Meta-Analysis. Soc. Sci. Med. 1997, 44(9): 1325-1339.
23. World Health Organization. Integrated Management of Cardiovascular Risk. Report of a WHO Meeting. Geneva, 9-12 July 2002, Noncommunicable Diseases and Mental Health, World Health Organization.
24. Lichtenstein E, Nettekoven L, Ockene JK. Community Intervention Trial for Smoking Cessation(COMMIT): Opportunities for Community Psychologists in Chronic Disease Prevention. Am J Community Psychol. 1991, 19(1):17-39.
25. Shintani T, Beckham S, O’Connor HK, Hughes C, Sato A. The Waianae Diet Program: A Culturally Sensitive, Community-based Obesity and Clinical Intervention Program for the Native Hawaiian Population. Hawaii Med J. 1994, 53(5): 136-141,147.
26. Wechsler H, Wernick SM. A Social Marketing Campaign to Pomote Low-fat Milk Consumption in an Inner-city Latino Community. Public Health Reports. 1992,107(2): 202-207.
27. Hankey GJ. Risk Factor Management to Prevent Stroke. Ischemic Stroke: Advances in Neurology. Vol.92. Edited by H.J.M Barnett, Julien Bogousslavsky, and Heather Meldrum. Lippincott Williams & Wilkins, Philadelphia 2003.
28. Ebrahsim, S, Davey Smith, G. Multiple Risk Factor Intervention for Primary Prevention of Coronary Heart Disease. The Cochrane Library, Volume(1).2003.
29. Jousilahti P, Tuomilehto, J, Korhonen, HJ, Vartiainen E, Puska P, Nissinen A. Trends in Cardiovascular Disease
Risk Factor Clustering in Eastern Finland: Results of 15-Year Follow-Up of the North Karelia Project. Preventive Medicine. 1994, 23: 6-14.
30. Puska P. Nutrition and Mortality: the Finnish Experience. Acta Cardiol. 2000, 55(4): 213-220.
31. Schmid TL., Pra M, Howze E. Policy as Intervention: Environmental and Policy Approaches to the Prevention of Cardiovascular Disease. American Journal of Public Health. 1995, 85(9): 1207-1211.
32. World Health Organization. Secondary Prevention of Noncommunicable Diseases in Low- and Middle-Income Countries Through Community-Based and Health Service Interventions. World Health Organization-Wellcome Trust meeting report 1-3 August 2001.
33. Jolliffe JA, Rees k, Taylor RS, Thompson D, Oldridge N, Ebrahim S. Exercise-based Rehabilitation for Coronary Heart Disease. Cochrane Data Syst Rev. 2001, (1):CD001800.
34. Kuulasma K, Tunstall-Pedoe H, Dobson A, Fortman S, Sans S, Tolonen H et al. Estimation of contribtion of changes in classic risk factors trends in coronary-event rates across the WHO/MONICA Project population. Lancet 2000, 355(920s):675-687.
35. Tunstall-Pedoe H, Vanuzzo D, Hobbs M, Mahonen , Cepaitis Z, Kuulasma K, Keil U. Estimation of contribution of changes in coronary care to improving survival, event rates, and coronary heart disease mortality across the WHO/MONICA Project populations. Lancet, 2000, 355(920s):688-700.
36. The WHOQOL Group. The World Health Organization Quality of Life Assessment(WHOQOL): Position Paper from the World Health Organization. Soc. Sci. Med. 1995, 41(10):1403-1409.
37. Spilker B. Quality of Life and Pharmacoeconomics in Clinical Trial(second edition). Lipincott-Raven Publishers 1995.
38. World Health Organization. The World Health Report 2002: Reducing Risks, Promoting Healthy life. Geneva, World Health Organization.
39. Oberman A, Kuller Lh, Carleton RA. Prevention of Cardiovascular Disease---Opportunities for Progress. Preventive Medicine. 1994, 23:
727-732.
40. World Health Organization. Life Course Perspectives on Coronary Heart Diseases, Stroke and Diabetes. Summary Report of a Meeting of Experts 2-4 May 2001, Noncommunicable Diseases and Mental Health Cluster, World Health Organization.